Knee Replacement Decision Calculator
How Ready Is Your Knee for Replacement?
This tool helps you evaluate your knee condition against clinical criteria discussed in the article. Enter your values below to see if you meet the typical thresholds for knee replacement consideration.
Your Knee Replacement Assessment
Key Thresholds Met
What these scores mean
- 0-2 points Not typically a surgical candidate
- 3-4 points Consideration for replacement
- 5-6 points Strong candidate for replacement
When you’re wondering Knee Replacement a surgical procedure that swaps damaged joint surfaces with artificial components with a new one, the answer isn’t a simple “yes or no.” Your knee has to hit certain pain and function thresholds before doctors usually recommend the operation.
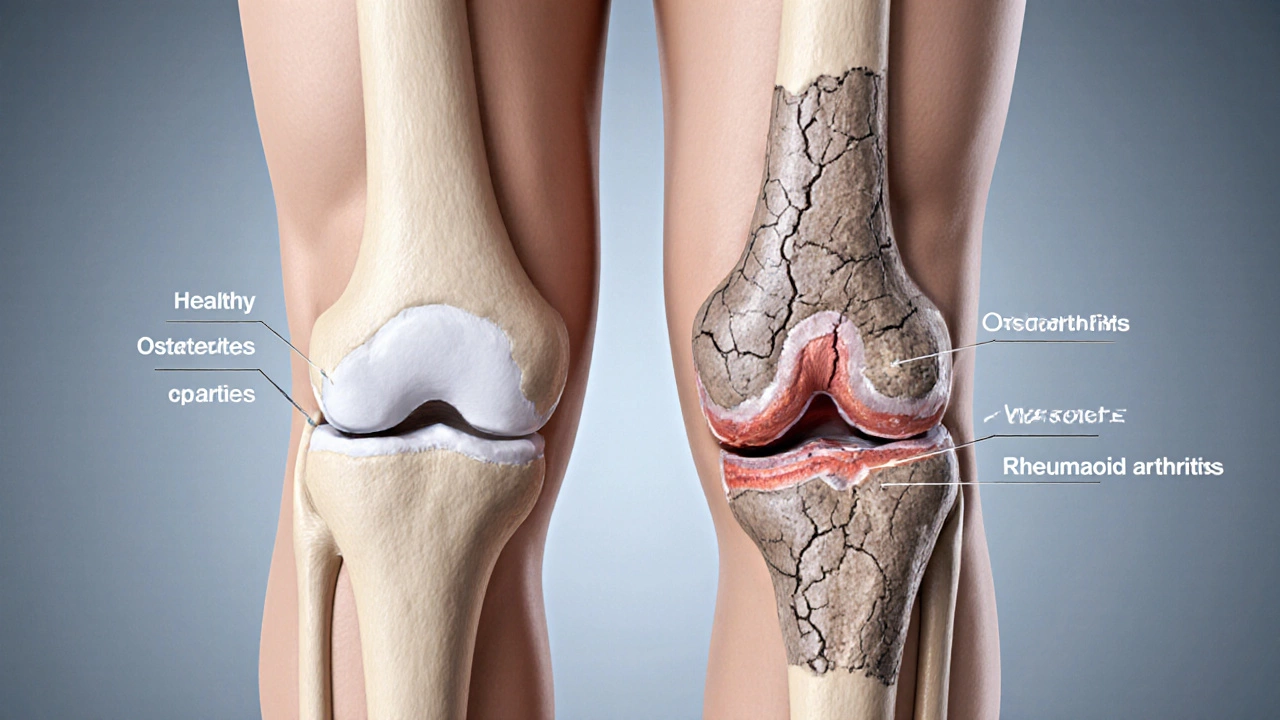
What actually wears out a knee?
Most people end up needing a joint swap because the cartilage - the smooth cushion that lets the femur glide over the tibia - deteriorates over time. The two biggest culprits are:
- Osteoarthritis a wear‑and‑tear arthritis that gradually erodes cartilage
- Rheumatoid arthritis an autoimmune disease that inflames the joint lining and can destroy cartilage quickly
Both conditions turn a smooth joint into bone‑on‑bone friction, leading to pain, swelling, and loss of movement.
When do non‑surgical options stop working?
Before anyone pulls the trigger on surgery, most orthopedists will try a lineup of conservative treatments:
- Physical therapy to strengthen surrounding muscles and improve gait.
- Weight management - excess body mass adds extra load to the joint.
- Pain‑relieving medication, from NSAIDs to occasional steroids.
- Injectable options like hyaluronic acid or platelet‑rich plasma.
If after 3-6 months of these measures your pain still spikes during daily activities, it’s a sign the knee has reached a critical point.
Clinical red flags that push surgeons toward replacement
Doctors use a blend of subjective reports and objective measurements. The most common decision factors are:
- Pain severity - typically measured on a 0‑10 visual analog scale. Scores of 7 or higher at rest, or 5+ during light activity, are strong indicators.
- Functional limitation - inability to walk more than 300 m, climb stairs, or sit cross‑legged without sharp pain.
- Radiographic grading - X‑ray imaging (see box below) that shows joint space narrowing of less than 2 mm or severe bone spur formation.
- Range of motion (ROM) - loss of flexion below 90° or extension lag greater than 5°.
- Joint stability - tests that reveal laxity or shifting of the tibia on the femur.
- Body Mass Index (BMI) - a BMI over 35 kg/m² raises complication risk, but it doesn’t automatically rule out surgery; it just pushes the conversation toward weight loss first.
When three or more of these criteria line up, most surgeons consider the knee “ready” for replacement.
How doctors evaluate the knee - the checklist
| Assessment | What It Shows | Typical Threshold |
|---|---|---|
| Patient‑reported pain (VAS) | Subjective discomfort level | ≥7 at rest or ≥5 with activity |
| Functional score (KOOS/ WOMAC) | Ability to perform daily tasks | Score ≤ 50 % of age‑adjusted norm |
| Radiographs (AP, lateral, sunrise) | Joint space width, osteophytes, alignment | Space < 2 mm; severe osteophytes |
| Range of Motion (goniometer) | Flexion/extension limits | Flexion < 90°, extension lag > 5° |
| Stability tests (Lachman, varus/valgus stress) | Ligament integrity | Significant laxity or subluxation |
| BMI calculation | Weight‑related risk factor | > 35 kg/m² (consider weight loss first) |
These numbers aren’t carved in stone, but they give both you and your surgeon a clear picture of where the knee stands.
Partial vs. Total Knee Replacement - which is right?
If the damage is confined to one compartment (usually the inside or outside of the knee), a Partial Knee Replacement also called unicompartmental knee arthroplasty, replaces only the worn compartment may be enough. Otherwise, a Total Knee Replacement replaces the entire joint surface with metal and plastic components is the standard.
Here’s a quick side‑by‑side comparison:
| Feature | Partial (Unicompartmental) | Total (Arthroplasty) |
|---|---|---|
| Indicated when | Damage limited to one compartment | Widespread damage across two or three compartments |
| Recovery time | Approx. 6‑8 weeks for normal activities | 3‑6 months for full recovery |
| Range of motion outcome | Often closer to pre‑injury levels | Very good, but may lose a few degrees of flexion |
| Long‑term survivorship | 10‑15 years, depending on activity level | 15‑20 years or more with modern implants |
| Potential for future surgery | If arthritis spreads, conversion to total may be needed | Usually definitive, though revision is possible |
Both options aim to eliminate pain, but the choice hinges on the pattern of wear you see on the X‑ray and the surgeon’s assessment of ligament health.
Preparing for the day of surgery
Once you and your orthopedist agree that surgery is the next step, the pre‑op checklist looks something like this:
- Medical clearance - blood work, heart evaluation, and anesthesia consult.
- Pre‑hab - a short‑term, targeted Physical Therapy program to strengthen quadriceps and improve knee ROM before surgery.
- Medication review - stopping blood thinners or certain supplements a week before.
- Home setup - arrange a safe space, a recliner, and a sturdy walking aid.
- Post‑op plan - schedule follow‑up visits, arrange for a caregiver, and understand pain‑management protocol.
Following these steps can shave weeks off your recovery and reduce the risk of complications.
Recovery realities - what to expect in the first months
Most people walk with a cane or walker by day three. Physical therapy becomes a daily habit:
- Weeks 1‑2: Gentle range‑of‑motion exercises and quad sets.
- Weeks 3‑6: Progress to stationary bike, light resistance bands, and short walks.
- Months 3‑6: Full weight‑bearing, low‑impact activities like swimming or cycling.
By six months, the majority report pain scores under 2 on the VAS and can resume most hobbies, though high‑impact sports may still be discouraged.
Common myths that cause confusion
Let’s bust a few lingering doubts:
- Myth: “If I’m 70, I shouldn’t get a knee replacement.” - Fact: Age isn’t a barrier; health status and activity goals matter more.
- Myth: “All knee replacements last forever.” - Fact: Implants can wear out after 15‑20 years, especially in very active patients.
- Myth: “I’ll be on crutches forever.” - Fact: Most people stop using assistive devices within 6‑8 weeks.
Quick reference guide - is it time for a replacement?
Use this cheat‑sheet the next time pain hits:
| Indicator | Threshold | Interpretation |
|---|---|---|
| Pain VAS (rest) | ≥7 | Strong surgical candidate |
| Walking distance | <300 m without stop | Consider replacement |
| Joint space on X‑ray | <2 mm | Significant cartilage loss |
| Flexion ROM | <90° | Functional limitation |
| BMI | >35 kg/m² (if no weight‑loss effort) | Weight‑loss first, then reassess |
If you tick at least three boxes, schedule a visit with an orthopedic surgeon. They’ll run the full checklist, discuss partial vs. total options, and map out a personalized plan.
How long does a knee replacement surgery take?
The operation itself usually lasts 60‑90 minutes for a total knee replacement and 45‑60 minutes for a partial one. Anesthesia and pre‑op prep add another hour or so.
Is knee replacement painful after the surgery?
You’ll feel soreness for the first few weeks, but pain is usually manageable with oral meds and occasional nerve blocks. By the third month most patients report minimal discomfort.
Can I get a knee replacement if I’m overweight?
Being overweight raises the risk of infection and implant wear, but surgeons often proceed after a short‑term weight‑loss program. The key is to lower BMI below 35 before the incision.
What’s the lifespan of a knee implant?
Modern implants can last 15‑20 years or more, especially when patients avoid high‑impact sports and maintain a healthy weight.
Will I need rehab after a knee replacement?
Yes. A structured rehab program is essential for regaining strength and range of motion. Most people attend physical therapy 2‑3 times a week for the first six weeks.
Bottom line: You don’t need to wait until the knee is completely useless. Once pain, function, and imaging line up with the thresholds above, a replacement can give you a pain‑free, active life again.